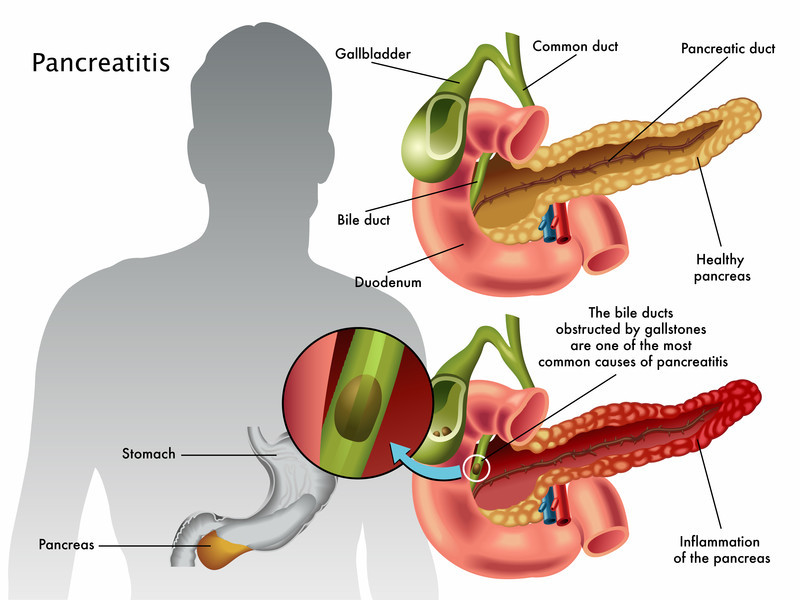
What is Chronic Pancreatitis?
Chronic pancreatitis is a progressive inflammation of the pancreas that leads to long-term damage, causing severe abdominal pain, digestive issues, and impaired insulin production. Over time, the pancreas loses its ability to function properly, affecting the body’s ability to digest food and regulate blood sugar levels.
When medication and lifestyle changes fail to control symptoms, surgical intervention becomes necessary to relieve pain, improve digestion, and enhance quality of life.
When is Surgery Needed for Chronic Pancreatitis?
Surgery is considered when:





Surgical treatment can provide significant symptom relief, prevent complications, and improve digestion and insulin regulation.
Types of Surgery for Chronic Pancreatitis
There are several surgical options depending on the severity and nature of the condition:
1. Pancreatic Drainage Procedures
If pancreatic ducts are blocked due to stones or narrowing, procedures like lateral pancreaticojejunostomy (Puestow Procedure) help drain the pancreas by connecting it to the small intestine, relieving pressure and pain.
2. Pancreatic Resection (Partial Pancreatectomy)
For patients with localized damage or chronic inflammation in specific areas of the pancreas, the damaged portion of the pancreas is removed, preserving the rest of the organ’s function.
3. Total Pancreatectomy with Islet Autotransplantation (TP-IAT)
For severe cases where the entire pancreas is diseased, total removal may be necessary. In some cases, islet autotransplantation helps retain insulin-producing cells to reduce the risk of diabetes.
4. Whipple Procedure (Pancreaticoduodenectomy)
If chronic pancreatitis affects the head of the pancreas, the Whipple procedure removes the affected portion along with part of the small intestine and bile duct, ensuring pain relief and digestive improvement.
Each procedure is tailored to the patient’s condition, ensuring optimal outcomes with minimal complications.
Benefits of Surgery for Chronic Pancreatitis
Surgery for chronic pancreatitis offers several life-changing benefits, including:





What to Expect Before & After Surgery?
Before Surgery
- Medical Evaluations – Imaging tests (MRI, CT scan) and blood tests to assess the severity.
- Fasting & Medication Adjustments – Pre-surgery dietary and medication instructions.
- Personalized Surgical Plan – Dr. Ankur V. Tiwari Gastro Surgeon prepares a customized treatment approach based on your overall health and surgical needs.
After Surgery
- Hospital Stay – Typically 3-7 days depending on the procedure.
- Pain Management – Controlled with medications and gradual activity resumption.
- Dietary Changes – A soft diet initially, progressing to normal food intake.
- Follow-Up Care – Regular checkups ensure proper healing and function recovery.
Recovery varies depending on the type of surgery performed, but most patients experience substantial improvement within weeks.
1. What is chronic pancreatitis and how does it affect normal people?
Chronic pancreatitis is a long-term inflammation of the pancreas that gradually damages the organ’s ability to function properly. In normal people, it can cause persistent abdominal pain, indigestion, weight loss, and diabetes if not treated on time. Early diagnosis and expert care help manage symptoms and prevent complications.
2. What are the common symptoms of chronic pancreatitis?
Upper abdominal pain that may spread to the back
Nausea and vomiting
Unexplained weight loss
Greasy or oily stools (steatorrhea)
Signs of diabetes due to reduced insulin production
If you experience these symptoms, consult Dr. Ankur V. Tiwari, an experienced Surgical Gastroenterologist in Vadodara, for proper evaluation and treatment.
3. What are the main causes of chronic pancreatitis?
The most common causes include:
Excessive alcohol consumption
Gallstones and bile duct problems
High triglyceride levels
Genetic or autoimmune conditions
Previous episodes of acute pancreatitis
Identifying the cause early allows for better treatment planning and prevents further pancreatic damage.
4. How is chronic pancreatitis diagnosed?
Diagnosis involves a combination of:
Blood tests to assess pancreatic function
Imaging tests like ultrasound, CT scan, or MRI
Endoscopic procedures for detailed evaluation
At Aadicura Superspeciality Hospital, advanced diagnostic facilities ensure accurate assessment and personalized care.
5. What are the treatment options for chronic pancreatitis?
Treatment depends on the severity and underlying cause:
Lifestyle changes – Avoid alcohol, quit smoking, and follow a low-fat, pancreatic-friendly diet
Medications – Pain management, enzyme supplements, and diabetes control
Endoscopic or surgical procedures – For severe cases involving bile duct blockages, pseudocysts, or pancreatic stones
Regular monitoring – To manage long-term complications effectively
With timely intervention by experts like Dr. Ankur V. Tiwari at Aadicura Superspeciality Hospital, most patients experience significant symptom relief and improved quality of life.
